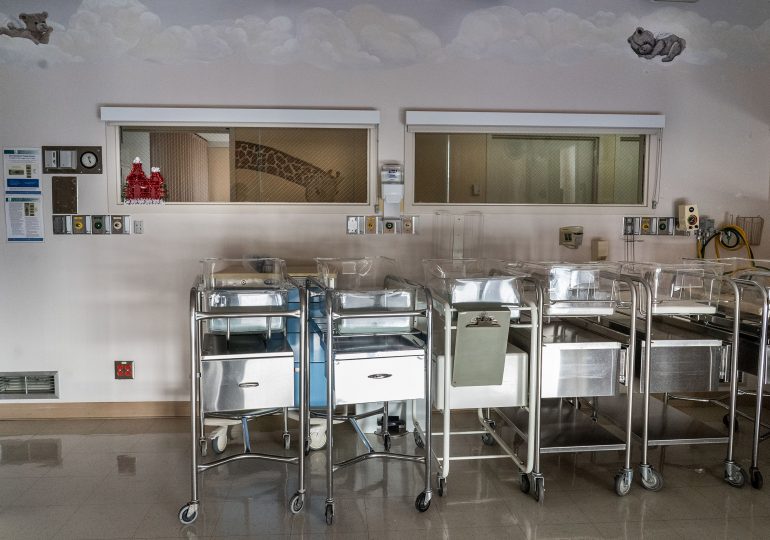
Dr. Jesanna Cooper cried when she heard that the labor and delivery unit at Princeton Baptist Medical Center in Birmingham, Ala., would close in October 2023. She’d started delivering babies at the hospital in 2013, and had helped make it one of the best maternity care centers in the U.S., a huge accomplishment in a state with one of the highest rates of maternal mortality.
[time-brightcove not-tgx=”true”]
Princeton Baptist is located in a low-income part of Birmingham where birthing mothers often had serious complications. But Cooper and her partners in private practice worked with the hospital to bring in midwives, reduce the number of C-sections, and lower the amount of obstetric trauma women experienced. “We realized that we could really change an entire community’s health trajectory,” she says.
Yet Cooper left the practice in December 2022 after getting burned out. The next fall, Brookwood Baptist Health, which owns the hospital, said it was discontinuing ob-gyn programs at Princeton and another Alabama hospital to “allow these hospitals to focus more strongly on the services their patients trust them to provide.” These were two of the hundreds of maternity wards to close across the U.S. in recent years—more than 217 since 2011, according to the health care consulting firm Chartis, leaving many women in regions without care. Tenet Healthcare, which owns Brookwood, did not return multiple requests for comment from TIME. But doctors and analysts say there’s little mystery why providers shutter labor and delivery units: they make comparatively little money, and, in some cases, they lose a lot of it.
“Average reimbursement for obstetric care turns out to be quite low, if compared to other types of services,” says Caitlin Carroll, a professor at the University of Minnesota who studies health economics and hospital closures. “So hospitals are closing their labor and delivery units because they tend to be unprofitable.”
Few hospitals have said as much publicly. But hospital administrators have indicated in interviews with academics that labor and delivery units are often in the red. For a long time, the field has been known as a “loss leader,” meaning it loses money but might bring in new business as families who delivered at a hospital return there for care. Private practices are struggling too, with ob-gyn providers leaving the profession. Cooper was the only ob-gyn at her private practice for six of the 10 years she was there, which meant she was on call 24/7. She tried to recruit a partner to join her but the pay was too low and hours too grueling, she says.
There are a number of reasons why the U.S. health care system is falling short when it comes to maternity care. All of them are about money. Insurance reimbursement rates are set in large part by a committee that critics say undervalues ob-gyn care relative to other, high-profit specialties.A large proportion of births in the U.S. are reimbursed through Medicaid, which pays hospitals less than other insurers. Because of the way billing codes are structured, pay for maternity care is often made in a lump sum meant to cover a woman’s whole pregnancy, which doctors say significantly under-prices the care they give. And some private insurers have gained near-monopolies in some states, shrinking competition and doctors’ ability to negotiate. Obstetrics also has among the highest rates of malpractice suits, which drives up insurance costs and pushes doctors away from the field. Taken together, the increasingly profit-driven business of health care has little incentive to focus on what is the most important moment in many people’s lives.
The irony of closing maternity wards isn’t lost on Cooper, who met me in a barbeque restaurant in Birmingham where she spotted a young child who had been delivered on her watch. The act of bringing a baby into the world is one of the most important things we do as a society—a matter of the survival of our species—but our health care system, as she laments, does not compensate for the work in line with its value. “How is it that we got paid $1,000 for nine months of prenatal care, labor and delivery, and postpartum care, but one hour of a joint replacement gets paid $1,600?” Cooper asks, referring to Alabama’s Medicaid compensation rates.
The low compensation rates for labor and delivery have big implications for U.S. maternal and fetal outcomes. As maternity wards close, women have to travel further for care, making it more difficult to both make their normal appointments and to get to the hospital in time once they go into labor. About half of women who live in rural areas must travel more than 30 minutes to an obstetric hospital, according to the March of Dimes. This leads to a 9% increase in the probability of maternal deaths or a severe health episode compared to women in areas with greater access, the March of Dimes finds. Black women already have higher rates of death and complications in birth than do white women, yet 1 in 6 Black babies in 2022 were born in areas of limited or no access to maternity care.
There are two big costs when a woman delivers a baby. The first is what her doctor gets paid for care. Then there’s the fee paid to the hospital for facilities, equipment, and staffing. Hospital fees can be quite high, because maternity wards have to be staffed every hour of the day, every day of the year, with access to operating rooms and anesthesiologists. A doctor’s fees for maternity care—what Cooper got paid—are often compensated through what’s called a “global fee,” which is essentially a lump sum to cover prenatal appointments, labor and delivery, and the first 60 days postpartum.
Policymakers switched to bundled payments like this in the 2010s in an effort to reduce costly and unnecessary medical interventions. But rates have not kept pace with inflation and do not cover important services like maternal mental-health screening, says Joy Burkhard, policy director of the Policy Center for Maternal Mental Health, a nonprofit think tank. The global fee is derived from examples of an uncomplicated pregnancy, delivery, and postpartum care.
“The global fee needs to change,” says Lisa Satterfield, the senior director of health economics at the American College of Obstetrics and Gynecologists (ACOG), which is advocating for payers to unbundle different services provided at birth to increase doctor compensation. “It was meant to do good and has not.”
That the use of one billing code can wreak so much havoc on ob-gyn practices highlights a huge problem with the U.S. medical system: doctors are not paid for outcomes, but rather for performing a service. Because of the way we value those services, doctors who do some of the work that you’d think society considers most vital are in some cases losing money, and in others just breaking even.
In 1992, after a Congressional commission reviewed increasing physician pay and recommended a change in how compensation was calculated, Medicare transitioned to a system that pays physicians based on what’s called “relative value units” (RVUs). RVUs calculate how much skill and time is required for different procedures. Every few years, the American Medical Association’s (AMA) Specialty Society Relative Value Scale Update Committee, a group of doctors and health care professionals known colloquially as the RUC, updates RVUs. The Centers for Medicare and Medicaid Services then uses these RVUs as one of their inputs in setting rates. Private insurers also use the RUC to help determine their compensation rates.
Some doctors believe the RUC undervalues services for women because of the legacy of sexism in medicine. “When you compare anatomically similar RVUs between a variety of different surgeries, you’ll see that gynecologic surgery typically falls short in terms of reimbursement,” says Louise King, an ob-gyn and professor at Harvard Medical School, and the co-author of a paper that argues that care by women doctors and care for women are compensated at lower rates than care for men.
An academic study after the 1992 change found that “significant gender bias exists in Medicare reimbursement for female-specific services.” The government tried to raise rates for gynecological procedures, but a 1997 study found that in 80% of similar procedures, male services were still paid at a higher rate than female services. A similar 2015 study found that on average, male-specific cases have 27% higher reimbursement rates than female ones.
A big problem, says King, is that the RUC is made up of doctors from different specialties, but obstetrics and gynecology together only get one vote. When the ob-gyn on the RUC advocates for increases in billing for women’s care, they are often overruled by people in other specialties who perform similar procedures and may value their own work more highly. “Ob-gyn is kind of the stepchild and gets low priority” on the RUC, says Eric Christensen, research director at the Harvey L. Neiman Health Policy Institute.
Other analysts and industry groups reject the argument that sexism and the RUC are part of the problem. Very few specialties have more than one seat on the RUC, says David Chan, a Stanford professor who has studied price setting and the RUC. Doctors from just about every branch of medicine think they should be getting paid more. And there’s no one better to determine compensation than doctors who perform different procedures and know what they’re worth, Chan says.
ACOG and the American Medical Association also dispute that the RUC is leading to lower pay for ob-gyns. ACOG and the American Urological Association recently completed a joint analysis and found there was no “marked disparity in the value of services performed on women compared to similar services performed on men,” according to the American Medical Association. Satterfield, of ACOG, says that the group examined how billing codes have evolved over time and that gender-specific disparities have faded.
There are other reasons why maternity care struggles. One of the biggest is that ob-gyns have a large share of patients on Medicaid, the program that provides health insurance for low-income adults and children and people with disabilities. Though you can qualify for Medicaid if you are a parent, your income has to be quite low; if you are pregnant, your income can be much higher. Medicaid currently finances about 41% of births in the U.S.
Medicaid reimbursement falls significantly short of a doctor’s costs of providing a service—so much so that many private practices don’t accept Medicaid. “If your facility treats a large share of Medicaid patients, you are in a tough spot because reimbursement is so poor,” Christensen says. Doctors receive just $1,690 for that nine or so months of pregnancy care for Alabama Medicaid patients, according to state fee schedules. A hip joint replacement—a procedure that takes just a few hours—would be compensated at a rate of $1,617, according to the same fee schedule. (Alabama Medicaid did not respond to multiple requests for comment, except to say that information about Medicaid fees would come from an Alabama Open Records Law request. In Alabama, only residents are allowed to submit such requests.)
Medicaid reimbursements to providers vary by state. Compensation for an identical office visit ranged from $37 in Minnesota to $160 in Alaska in 2009, according to Diane Alexander, a professor at the Wharton School at the University of Pennsylvania who studies health care economics. Alexander compiled state Medicaid fee-for-service reimbursements for obstetric and gynecologic procedures between 1990 and 2012 and found that in some states, including Alabama, compensation for pregnancy and delivery care actually decreased over that time period.
The federal government has some influence in Medicaid policy. A spokesperson for the Centers for Medicare & Medicaid Services (CMS) told TIME in an email that CMS is trying to enhance maternity care delivered to enrollees. But states establish their own payment rates within federal requirements. While states have to ensure that Medicaid payment rates are “efficient, economic, and sufficient” so that providers will participate, the spokesperson said, they are only required to do so “to the extent that such care and services are available to the general population in the geographic area.”
Medicaid and the global fee are two reasons that ob-gyns are leaving the profession. But there are others. Private insurance in some states has low reimbursement rates because one insurer effectively has a monopoly on the market, making it difficult for doctors to negotiate. In Alabama, for instance, Blue Cross Blue Shield of Alabama provides insurance to about 96% of Alabama residents who get their insurance from a large employer. When there’s just one insurer, it is much more difficult for hospitals to negotiate higher rates, says Cooper. “You get paid what you get paid. It’s not like you can negotiate that,” she says. “There’s no competition.” (Blue Cross Blue Shield of Alabama said in a statement to TIME that its data indicates its labor reimbursement rates are “in line” with other health insurers in the Southeast.)
Obstetrics also has one of the highest rates of medical-malpractice insurance, making practicing more expensive than in other fields. Around 64% of ob-gyns have been sued, according to an American Medical Association study, compared to, for example, just 16% of psychiatrists and 17% of pediatricians. The rate of litigation led many ob-gyns to reduce the number of deliveries they perform or decrease the number of high-risk patients they accept, according to the ACOG.
One solution would be to move away from a fee-for-service model overall and pay doctors for outcomes rather than for what procedures they perform. Some hospitals have tried in the last decade, says Elizabeth Cherot, the president of the March of Dimes, which studies health outcomes. “If you work towards outcomes instead of fee-for-service, you have a much more equitable model.”
After her practice closed, Cooper started working at an obstetrics emergency room in Montgomery, Ala. She says she sees extremely sick patients come to the emergency room to give birth because they live in a place where there’s no maternity ward. One woman, Cooper recalls, gave birth in a rural emergency room without an ob-gyn and was transferred to Cooper’s hospital with her newborn, whom no one had thought to feed after birth, because the hospital was not accustomed to handling childbirth.
“These doctors are just incredibly busy and don’t have the time for personal communication and support that we did at Princeton,” Cooper says. “If you are one person and you have a lot of people you are trying to not have die, you are not thinking about an empowering birth experience.”
Yet the economics of the health care system means that high-volume maternity wards are becoming more common. A hospital with a birth every now and then can’t make it work financially. Consolidation seems to be what many hospitals and physician groups are doing to try and maintain ob-gyn service. That’s despite the fact that the Biden Administration is trying to lower maternal mortality rates by urging more hospitals to operate the kind of maternity ward that Jesanna Cooper helped build in Birmingham. Last November, the Biden Administration launched a “birthing-friendly’ designation to help patients identify hospitals and health systems that are helping to improve maternal and infant health. Many of the factors that it uses to judge whether a hospital is birthing-friendly are the same one that Cooper used for her practice: high breast-milk feeding rates, low c-section rates, and high VBAC (vaginal birth after cesarean) rates.
Those types of things make a big difference to women. Rauslyn Adams gave birth to her first child at a high-volume teaching hospital that was very impersonal, she says. Adams gave birth to her second child at Princeton. “The experiences were night and day,” she recalls. At Princeton, she was encouraged to come up with a birthing plan, worked with midwives who helped her achieve the experience she sought, and had a support group of other mothers who made her prenatal and postpartum experience much more comfortable.
Like Cooper, Adams cried when she heard that Princeton was closing. “It was like a slap in the face to Black women,” says Adams, one of the founders of Chocolate Milk Mommies, a Birmingham lactation-support group. “It was as if they said, ‘How dare you have a wonderful peaceful birthing experience and high lactation rates. We’re closing it down.’”
Even more frustrating for many in Birmingham is that Cooper dramatically increased volumes at Princeton’s labor and delivery unit in her time there, delivering about 30 to 40 babies a month at the point of the unit’s closure—about triple the volume it had once done, bringing in many more private insurance patients, who earn more money for the hospital. It still wasn’t enough to convince Brookwood to keep the L&D ward open—the group consolidated three labor and delivery units into one.
What Cooper discovered, she says, is that it doesn’t work financially to give women the kind of care they want during childbirth and that she wanted to provide. To get low c-section rates, you might have to set aside a room for a woman to labor in for 48 hours along with dedicated support staff to help her. That’s much more expensive than just performing a c-section—which happens to be a higher RVU, and pays more. “Hospitals aren’t incentivized to take that time,” she says. ”They have sick people that need those rooms.”
This article was produced as a part of a project for the USC Annenberg Center for Health Journalism’s 2023 Impact Fund for Reporting on Health Equity and Health Systems.
Leave a comment